Guest Editorials are by invitation and meant to provoke discussions on topics relevant to Fetal Radiology in India. Ideally, the topics focus on grey areas where there are no clear-cut answers or solutions to apply and that require in depth thought from the larger community. The aim is to bring these areas into a larger and wider discussion with the understanding that not every point is going to be agreeable to all. If it were agreeable to all, we do not need to discuss it. The opinions expressed in the editorials are the personal opinions of the author and may not reflect the official positions of organizations associated with the author.
Editor-in-Chief: Dr. Rijo Mathew Choorakuttil
Author: Dr. Prashant Onkar
Author Affiliations:
- Associate.Professor of Radiodiagnosis, NKPSIMS and LMH, Hingna Road, Nagpur-440018. E-mail: drprashantonkar@gmail.com.
- President, Maharashtra State Branch of IRIA,
- Member, PCPNDT Committee and
- Member, Fetal Radiology Outreach Program Committee of IRIA.
Introduction
Radiology is a diagnostic and therapeutic modality that has blossomed in last four decades. There is newer and better resolution of ultrasound (USG) images, which has increased its use to improve diagnosis of fetal conditions. Fetal imaging is now very well supported by genetic investigations. More disorders and fetal environmental changes are detected at early gestational age thereby helping in timely intervention and treatment.
Fetal radiology may be defined as a branch of radiology that studies fetal well being and conditions that affect the fetus using various radiological modalities and their treatment as needed.
The focus of diagnostic imaging in obstetrics comprises two major divisions. These include the evaluation of fetal well being and detection of abnormalities that may impact fetal wellbeing. Both are equally important to predict the outcome of pregnancy. A major consideration is the ability of ultrasound machines to identify preventable, treatable conditions like Fetal Growth Restriction (FGR) and to identify feto-maternal factors that may impact the well being of the fetus at an early gestational stage. This warrants the routine and regular use of ultrasound in antenatal care to assess fetal wellbeing throughout the course of pregnancy and plan for childbirth in certain conditions.
Indian scenario in general
The developed world has less density of population, lower birth rate, better maternal education and nutritional status with a lower incidence of FGR. Technology is available and accessible to the majority of the population and the focus is more on improving the detection of fetal abnormalities at earliest age. Globally,congenital anomalies affect 2–3% of births (1). Out of these, the incidence of chromosomal anomalies is a small proportion.In a study, the prevalence of chromosomal anomalies was 6.38 per 10,000 births (2).The detection of fetal abnormalities by USG needs hi tech costly equipment. Once suspicion of abnormality is raised by USG, further confirmatory investigations include invasive procedures and /or genetic screening. This is again significantly costly as well as a time-consuming affair. The reporting of some tests require few weeks and the mother and family is at tremendous stress for few weeks till final lab results are out.
India still leads in neonatal mortality rate (NMR) despite increase in rates of detection of congenital anomalies and rapid development in genetics and various investigations. In 2013, it was 28 per 1000 live births. Though there is decline in the NMR,still about 0.75 million neonates die every year in India.
The fetus is not able to achieve its intrinsic growth potential in Fetal growth restriction (FGR) or intrauterine growth restrictiondue to anatomical or functional disorders and diseases. More than 50% of low birth weight (LBW) infants born in India are FGR (3).If we go to the causes of Neonatal Mortality, nearly half of them are due to pre term complications and only around 8.5 percent are due to congenital abnormalities. (See Figure) Other causes include infections and intra-partum complications.
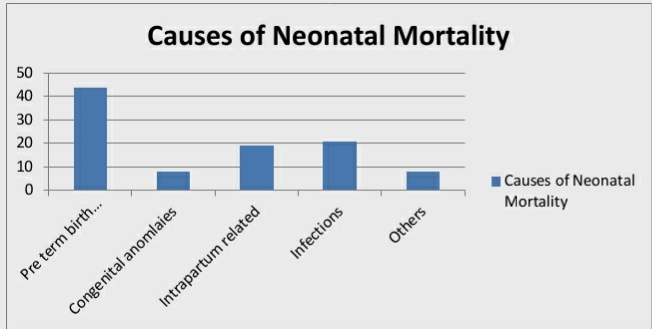
The rate of FGR in India vastly outnumbers the reported incidence of detection of abnormalities.If we compare the fatal or life limiting congenital anomalies with FGR, there are far more number of perinatal mortality case due to FGR.Nearly 30% of neonates that are born in India have a LBW (weight <2500 g) in India. About 60% of the LBW infants are born at term after fetal growth restriction, whereas the remaining 40% are born preterm (4). Community-based studieshave shown that LBW infants are at 11–13 times increased risk of dying than Normal Birth Weight infants. Indeed, >80% of total neonatal deaths occur among LBW/preterm neonates (5, 6, 7). The USG screening for FGR does not need sophisticated machines. The capital requirement is less and in same cost more machines can be available for screening more number of patients. Supporting a FGR pregnancy is less costly, more fruitful and effective if we consider the national scenario.
Maternal factors including age at birth, educational and nutritional status, and parity influence the fetal growth and thereby neonatal survival to a great extent.They have many acute neonatal problems that include perinatal asphyxia, hypothermia, hypoglycemia, and polycythemia. FGR babies are also likely to develop long term complications including growth retardation, major and subtle neuro-developmental handicaps, and developmental origin of health and disease (8).
The population growth rate in India is 1.14% per year as in 2018. So there are more than 1.5 crore live births every year. If we add still births, neonatal deaths, miscarriages and abortions many more conceptions occur every year. So the volume to be addressed is enormous and applying fetal radiology to this number of population is a huge task.
For Indian scenario ultrasound and other fetal radiology services can be categorized into Primary, Secondary, Tertiary and Referral level. We will discuss the issues at every level followed by possible solutions.
Primary
This is first step of health care services and usually taken care by government run primary health centers and sub-centers/wellness centers. They are manned by medical doctor or Auxiliary Nurse Midwife (ANM). Since 2016, under Pradhan Mantri Surakshit Matrutv Abhiyan (PMSMA) the Government of India has included at least one USG study to be done during each pregnancy (9). The government has empaneled various private clinics or trust hospitals for providing the USG services. The cost of INR 400 is borne by the government. This is supported by ANC check up by gynecologist/medical officer at designated date/interval. For the first time government has included ultrasound in primary obstetric care. This is an extremely welcome step towards enhanced ANC care. The ultrasound done under this scheme is a single point intervention. The population utilizing this level of care level lives in villages and is generally poor. Illiteracy, ignorance, poverty and distance of health care center from remote villages usually result in late reporting for ANC in the advanced gestational age. So the USG is done in second or third trimester or whenever the lady turns up at the primary care center.It is used for growth assessment without having previous dating data for interval growth or FGR assessment.
Knowing correct date of last menstrual period (LMP) is another important issue in India and most rural women really do not remember or keep records. Still one ultrasound in a pregnancy is expected to help many of the pregnancy in detecting gross FGR and useful for further follow up and management.
In first two years, only 1.5 million USG were done under PMSMA scheme (10). The initial figures are not encouraging as most of the population of pregnant women in India is absolutely not reached. A major cause for poor figures could be non-availability of USG facility at primary level and absence of radiologist/gynecologist at government hospitals.
Secondary
Secondary level of health care provides services to population located in smaller towns. They are catered by rural hospitals along with sub-district and district hospitals. In private sector, thousands of radiologists and/or gynecologist with small set-ups provide USG services. The population is less poor than rural as there are few employment opportunities available in these towns. Many of the rural hospitals in few states are equipped with ultrasound machines. In many states, this facility is not available at secondary level of care.The population in general avails services of the private Gynecology and Radiology set ups for routine scans and in emergency situation where government hospitals are unable to tackle them. As there is cost involved the use of USG is limited may be to one per pregnancy or only at gross FGR or emergency situations.
The private practitioner is not inclined for USG under PMSMA due to many reasons.One important major reason for non-takers for PMSMA is documentation pattern for every obstetric USG under the Pre Conception and Pre Natal Diagnostic Techniques act (PCPNDT). The process of PCPNDT compliance has been very complicated for the center owners. Having same form and formalities for invasive procedures and ultrasound examinations has resulted in double or triple record keeping. The quantum of USG examination is very huge. It becomes very time consuming for the center to complete the formalities. Every small error in record keeping is an offence under the act. There are thousands of cases filed under the PCPNDT act for minor deficiency in record keeping. No wise person is keen to increase workload and increase the chances of litigations. The fear of legal challenges for incomplete record usually works against desire of persons to contribute to the scheme. At some places government has tried to employ radiologist as part time at the secondary level hospitals. But the two-center norm i.e. under the act one radiologist/gynecologist can visit only two centers for doing ultrasound is proving detrimental.
Other reasons can be poor pay out, operational issues and at some places corruption issues.
Thus the key problem areas at secondary level areless available or non availability of USG facility at government set up and reduced uptake of PMSMA by practitioners.
Tertiary level
Tertiary level may constitute district or larger cities up to metro levels and include medical institutions, corporate hospitals and experts in fetal radiology who have special interest and experience. Usually the primary patients are from adjoining area along with referred cases from secondary level. Ultrasound and basic color Doppler machine are usually available in most of the government district hospitals. Again, availability of radiologist or gynecologist for doing ultrasound is a limitation. In the district hospitals and Government medical colleges where specialists are available, there is a huge workload of patients as they cannot deny services to anyone. Fetal USG exams are thus often restricted only to measurement of growth parameters due to paucity of time. The primary clientele of these hospitals is from low economic status where unfortunately the rate of FGR is more. Here the FGR is sometimes overlooked and under evaluated. But we can infer that every pregnant women can avail the USG facility. The detection of anomalies is the last priority. The patient being poor or ignorant is usually not concerned much in case anomaly is detected post natally. Due to high fertility rate, the value of live birth is very less in India especially in rural population.
Some government medical institutions are very well developed and offer package of quality services.
The private players like individual setups of fetal radiology experts and corporate are more focused and try to deliver an extra mile.They are organized in working and evaluation. They attempt to deliver every possible information about the pregnancy. These services are again costly and are used mainly by population having mid and high income. These are inaccessible to lower income strata which require it most. There is less number of such centers at this level.
Referral centers
Referral centers are very few and usually managed by corporate and expert individuals. The government institutions of national importance and few medical colleges also provide this level of care. The range of services include extremely advanced USG services, invasive procedures, genetic investigations and therapeutic procedures, genetic counseling, post-natal care and treatment etc. The team includes radiologist, gynecologist, geneticist, pediatrician, pediatric surgeon, counselor etc. Their role is confirmation of the diagnosis, further investigations and possible treatment. The patients availing these services usually have a precious pregnancy or complicated pregnancy. Most of the cases are referred from lower level of care. Majority of private center services are used by affluent population only. Very few public institutions are available for lower income group.
At this level, MRI is usually available as an additional tool for evaluation. MRI has shown potential in diagnosis of anomalies and their depiction as a whole. It does not have any role in FGR evaluation.
So, the problems at various levels are varied and require remedies as per their scale.
The possible remedies could be as under
- National program on fetal surveillance
Whenever the government has directly implemented any health program at all levels there has been improvement in health related statistics. We have experienced this in drives like polio, other vaccination, NRHM etc.
There should be National program on fetal surveillance including clinical examination, USG, invasive procedures, genetic investigations, nutrition,counseling etc.This can be supported by Wide publicity across all media for such facility (like immunization/pulse polio). This can be done by widespread implementation of PMSMA with above additional features to identify at risk population.The number of USG per pregnancy should be increased to two and three in due course of time. In pregnancy care the cost per patient is less but the number is very high. This will be an enormous task but if done shall be useful for healthy future generation. The IUGR babies are more prone to poor perinatal outcome and long term complications.It is understood that existing USG centers should have specialist and additional USG facilities at secondary level will be required to achieve the target. The private sector participation can be increased many fold by making favorable environment. The PMSMA has started the ball in motion to reach the goal. Like the popular health for all slogans, a “USG FOR ALL” drive is required.The machinery of NRHM shall be useful in implementation.
2. Inclusion of Doppler in active surveillance
As Doppler shows promising role in detection of early IUGR in first trimester itself Doppler should be included in the three USG scheme per pregnancy. There can be incentive for government doctor to take up USG. Additional training of doctors for Doppler is also required.
3. Establishment of uniform clinical and USG criteria
For fast and uniform evaluation of FGR or high risk for IUGR there has to be uniformity of various criteria. There are multiple tables and calculators available and most are from developed world. The Indian criteria or calculators are not yet available. The Indian Radiological and Imaging Association (IRIA) has started taking steps in developing them under the program SAMRAKSHAN (11). There are guidelines available for ANC clinical evaluation. Similarly, there should be specific guidelines for USG evaluation. The government should come up with uniform practicing guidelines for evaluation of anomaly and FGR. Point to point book containing exact methodology, guidelines, interpretation and grading charts, mobile app with risk calculators should be prepared.
We all know it is humanly impossible to detect each anomaly in every USG. There is need for classification of USG examination like limited USG, anomaly, cardiac, Doppler,fetal brain etc. The government / academic bodies / institution of national importance can work together and issue reporting guidelines for various level examinations. These guidelines or formats should have must be reported and may be reported points in each of the examination. Implementation of these guidelines and reporting formats should be made compulsory across government sector and private.The orientation of medical field towards standardization of reporting formats across country is required.
4. Revisions in the PCPNDT act
The act and rules therein should be revised to make the record keeping easy and quick. Hassle free record keeping is required to increase participation of private sector in this program. The two center norms and other clumsy rules should be changedto include and increase participation from private sector.
5. Cost of reimbursement
Under government PMSMA scheme the cost paid to the private sector needs to be sufficiently enhanced.
6. Six month ultrasound training course
The program shall require additional huge number of radiologist/gynecologist. Present post graduate education capacity is not enough to produce them in a short time. Under the PCPNDT act there is six month ultrasound training for MBBS doctors. Recently the government has proposed 50% reservation for government doctors. This should be increased to 100 % and exclusively made available only for government doctors. These doctors can serve a bond of 10 years to work in government sector. With availability of these doctors in short time, the government can employ them at existing USG facility at secondary level. Some can be employed at upcoming USG facilities at this level. Feasibility of mobile medical unit with USG at PHC level by state government on designated dates of the month can also be worked out.This may increase the work load at secondary level but shall be more acceptable to large number of population.
7. Patient transport facility
The government under National Rural Health Mission (NRHM) has facilitated transport services for the ANC for institutional delivery. This has increased the rate of institutional delivery significantly. Such facility should be available for Ante Natal Care (ANC) check up or USG.
8. ANC USG can be brought under PMJAY
Few OPD procedures like dialysis are already covered under Pradhan Mantri Jan ArogyaYojna (PMJAY). ANC USG can be brought under PMJAY. As PMJAY is expected to cover half of India’s Population such facility shall increase the range of USG services to ANC mothers.
9. Improving maternal education
Evidence demonstrates that improving maternal education is the most effective and proven strategy to improve neonatal survival. Kerala’s achievement of stabilizing population growth and low levels of infant and neonatal mortality is partly attributed to its high female education levels. This angle also needs consideration. (12, 13, 14)
10. Setting up tertiary and referral level centers
Side by side government should establish tertiary and referral level screening centers for anomaly detection, fetal interventions etc.
11. Setting up Government level genetic labs
Government has come up with centralized pathology labs in many states. Same can be enhanced for genetic testing. This shall reduce cost and increase accessibility to the deserving population. They should be part of the national program.
12. Removing regional imbalance.
The NMR is extremely variable in various states in India. There is need of extra efforts in many urbanized states like Chhattisgarh, Madhya Pradesh Uttar Pradesh, West Bengal, Jharkhand, Bihar etc.
13. Digital health record
This record system should be devised for use of government and private sector. This will ensure standardization of data and collaboration in two sectors.
14. Role of private players
The non-government players also need to gear up for the challenge and contribute by way of formulating their own uniform guidelines and reporting formats. They also should actively engage in research for developing data from India for growth assessment, Doppler parameters, evaluation of FGR, follow-up and evidence on utility of early diagnosis and intervention. The various measures like Samrakshan project by IRIA are very welcome and should be adapted by other professional organization and their members across India. Same shall be useful for the government to plan the national fetal surveillance program for FGR.
15. Anomaly detection and management guidelines
The congenital anomaly detection and management is another extremely important part ofUSG examination. The development of separate evaluation and reporting guidelines for various types of USG examination shall help the USG users to concentrate on this aspect in an organized manner. Judicious and apt use of NIPT and other markers in evaluation of chromosomal and other abnormalities is need of the hour to reduce fear among the patients.
Conclusion
India has witnessed improvement in neonatal health statistics after the implementation of NRHM. The numbers of home deliveries are significantly reduced. There is a reduction in the incidence of LBW over years. Even with the reduced rates we are far behind the target. Reaching the enormous number of pregnant women is really a challenging task. Apart from the PMSMA, the country has launched several new initiatives to improve maternal and neonatal health.
There is huge number of FGR leading to LBW births. Fetal radiology is complementing ANC care from primary to referral level. Many of the risk factors are now identifiable at early gestational age by USG. There is strong need to integrate fetal radiology in the national fetal surveillance program as a prime factor. This can be done by including USG for each trimester under modified PMSMA. Government needs to engage private sector actively in this voluminous task by reducing some legal road blocks and improving reimbursement rates. The secondary level of care has to be strengthened at government level. Identifyingmore and more women with the modifiable risk factors for FGR at early gestational age and their management will result in improvement in birth weight, reduction in NMR. This needs support by standardized evaluation and management criteria developed and implemented by government and private sector together. This could reduce the cost of post natal treatment, child morbidity or loss; psychological trauma, violence due to child death etc. Finally our aim for healthy future generation can be achieved to great extent.
References
- Dolk H, Loane M, Garne E. The prevalence of congenital anomalies in Europe. Adv Exp Med Biol. 2010;686:349–364. doi: 10.1007/978-90-481-9485-8_20.
- Xiao-Hui Zhang, Li-Qian Qiu, Ying-Hui Ye, Jian Xu. Chromosomal abnormalities: subgroup analysis by maternal age and perinatal features in zhejiang province of China, 2011–2015. Clin Med Insights Pediatr. 2016; 10: 67–83.
- Khadilkar AV, Parthasarthy LS. Fetal Growth Restriction and Cardiovascular Health Among Adolescents Indian Journal of Pediatrics. 2017; 47: 107-108.
- Lee ACC, Katz J, Blencowe H, Cousens S, Kozuki N, Vogel JP et al. National and regional estimates of term and preterm babies born small for gestational age in 138 low-income and middle-income countries in 2010. Lancet Glob Health 2013; 1: e26–e36.
- National Neonatal Perinatal Database. Report for the year 2002–03. Available at http://www.newbornwhocc.org/pdf/nnpd_report_2002-03.PDF
- Bang AT, Bang RA, Baitule S, Deshmukh M, Reddy MH. Burden of morbidities and the unmet need for health care in rural neonates—a prospective observational study in Gadchiroli, India. Indian Pediatr 2001; 38: 952–965.
- Chaudhari S, Bhalerao MR, Chitale A, Pandit AN, Nene U. Pune low birth weight study—a six year follow up. Indian Pediatr 1999; 36: 669–676.
- Sharma D, Shastri S, Sharma P. Intrauterine growth restriction: Antental and Postnatal aspects. Indian Pediatr 2015;52: 107-108.. doi: 10.4137/CMPed.S40070
- Accessed online from : http://www.nrhmhp.gov.in/sites/default/files/files/PMSMA-Guidelines.pdf
- Accessed online from https://pib.gov.in/PressReleaseIframePage.aspx?PRID=1517166
- Choorakuttil RM, Patel H, Bavaharan R, Devarajan P, Kanhirat S, Shenoy RS, Tiwari OP, Sodani RK, Sharma LK, Nirmalan PK. Samrakshan: An Indian radiological and imaging association program to reduce perinatal mortality in India. Indian J Radiol Imaging 2019;29:412-7
- Agha S, Carton TW. Determinants of institutional delivery in rural Jhang, Pakistan. Int J Equity Health 2011; 10(1): 1–12.
- Navaneetham K, Dharmalingam A. Utilization of maternal healthcare services in southern India. SocSci Med 2002; 55(10): 1849–1869.
- Ogunlesi TA, Ogunlesi FB. Family socio-demographic factors and maternal obstetric factors influencing appropriate health-care seeking behaviours for newborn jaundice in Sagamu, Nigeria. Mater Child Health J 2012; 16(3): 677–684.