Author: Avni KP Skandhan, Aster MIMS, Kottakkal, Kerala
INTRODUCTION
The detection of adnexal masses in pregnancy, which are often incidental findings, has increased with the increased use of ultrasonography. (1-4). The current incidence of adnexal masses during pregnancy is reportedly between 1 in 81 and 1 in 8000 pregnancies (5). Earlier, adnexal masses were under detected due to a lack of technological advancements with a low discovery rate (6). Most of patients with adnexal masses are asymptomatic; however, the adnexal mass may be complicated by torsion of the lesion, rupture of the cyst, bleeding into the cyst, infection of the cyst, or may cause an obstruction of labour (7). Of the adnexal masses, the incidence of ovarian malignancy is 1 in 1500–32 000 pregnancies (8). The ovarian masses are often borderline with a low malignant potential (7,9).
Ultrasound is the most commonly used imaging modality in pregnant women (10). There are stipulated guidelines for diagnosis and management of adnexal masses laid down by the American College of Obstetrics and Gynaecologists (ACOG); however, these apply for the non-pregnant patients and there are no definite guidelines for the adnexal masses in pregnant patients (11). Decision making is difficult considering the foetal and maternal safety in pregnant women with lesions that are complicated or demonstrate malignant features however rare they are (11).
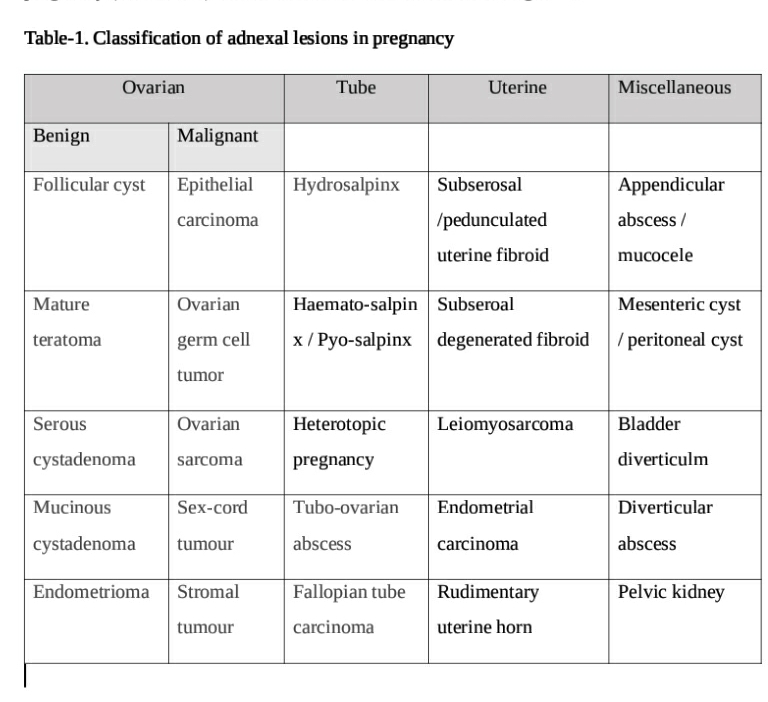
The predominant adnexal lesions are unrelated to pregnancy. The pregnancy related lesions are corpus leuteum cyst, ectopic pregnancy and theca leutein cysts (14). Lesions unrelated to pregnancy (see Table 1) can be classified based on source of origin (15).
IMAGING:
The predominant point of consideration in adnexal lesions during pregnancy are presence of complications and presence of imaging features of malignant potential. In such cases ultrasound serves to characterize the mass and to assess vascularity of the lesion and other emergent features (12). There are many categorization systems to characterise these lesions, the latest updated one is the Ovarian-Adnexal Reporting and Data System (O-RADS) (16). Proper use of these categorization systems helps us identify malignant risk features in adnexal lesions. (Figure 1, 2, 3 & 4). Based on O-RADS categorization, the suspicious features are:
- larger lesions (>10 cm),
- cysts with thick and irregular septations,
- cysts with irregular walls, papillary projections > 3 mm,
- lesions with solid areas having a higher vascularity (colour score), predominantly solid but lobulated and/or irregular lesions or
- ancillary findings such as ascites or omental nodules (16).
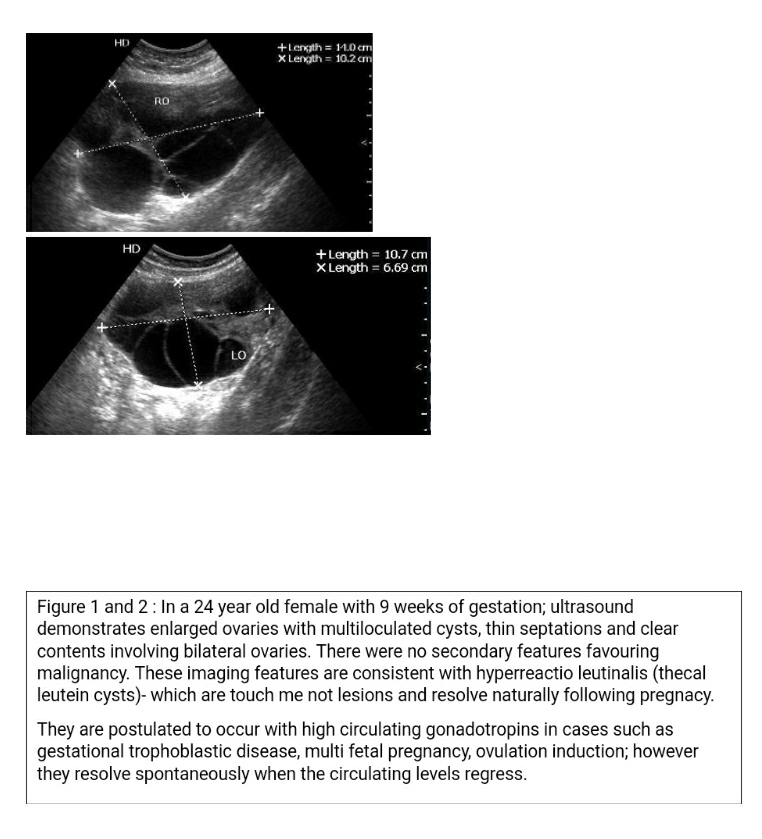
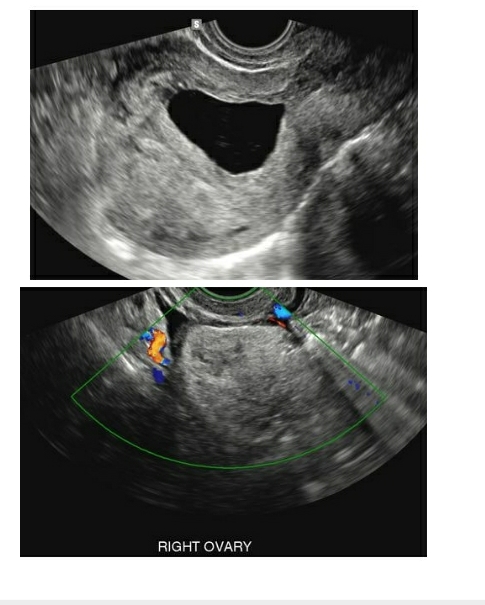
Image courtesy: Thank you Dr Alexandra Stanislavsky and Radiopaedia.
Image courtsey
When the ultrasound features are indeterminate, MR imaging can help to categorize the adnexal lesions better and help further management (17).
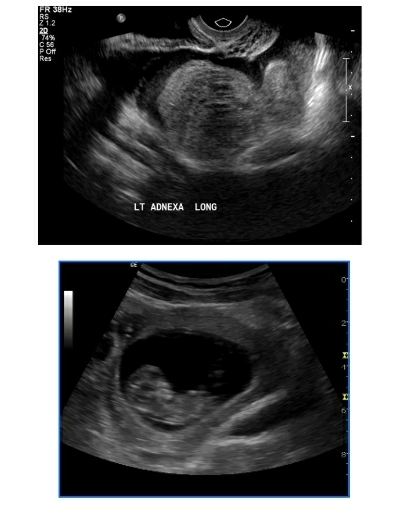
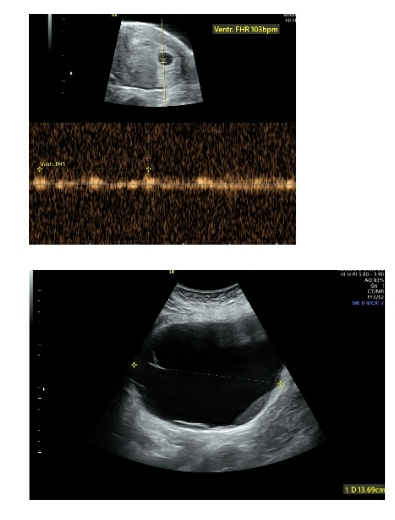
Ovarian torsion is another area where ultrasonography plays an important role especially when a patient presents with acute abdominal pain during pregnancy and an incidentally or otherwise known ovarian lesion (12). On a 2D scan, the lesions demonstrate an enlarged and oedematous ovary with a lesion within. In certain cases, it may be possible to see multiple tiny cystic structures arranged in the periphery, possibly follicles, pushed peripherally due to oedema (18) (Image: Figure 5 & 6). On further Doppler investigation there is either absent/poor or normal vascularity demonstrated based on the extent of the vascularity that is compromised (18, 19). The venous flow within the adnexa is the first to be compromised followed by the arterial flow (18). However, of all the Sonography and Doppler findings the most sensitive finding is the presence of a twisted vascular pedicle – whirlpool sign (20, 21, 22).
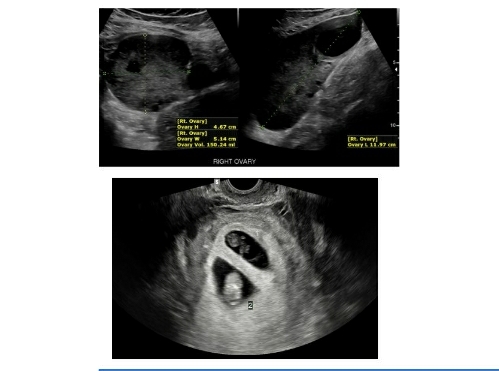
Image courtesy: Thank you Dr Alexandra Stanislavsky and Radiopaedia.
Cyst rupture is another encountered emergency secondary to an adnexal lesion in an otherwise healthy pregnancy. A rupture cyst, associated with hameoperitoneum and possibly a sentinel clot are the features found sonologically (23). ( Image : Figure 7 & 8)
CONCLUSION:
Adnexal masses during pregnancy have to be diligently investigated. Imaging forms an important part of the investigative procedure. Image characterisation can help delineate masses that are suspicious of malignancy and in further workup and management of these patients. Imaging helps us in the diagnosis of emergencies such as torsion or rupture of the lesion in whom an emergency surgical treatment is warranted.
REFERENCES:
- Yakasai I, Bappa L A. Diagnosis and Management of Adnexal Masses in Pregnancy. J Surg Tech Case Rep. 2012 Jul-Dec; 4(2): 79–85.
- Leiserowitz GS. Managing ovarian masses during pregnancy. Obstet Gynecol Surv. 2006;61:463–70.
- Glanc P, Salem S, Farine D. Adnexal masses in the pregnant patient: A diagnostic and management challenge. Ultrasound Q. 2008;24:225–40.
- Giuntoli RL, 2nd, Vang RS, Bristow RE. Evaluation and management of adnexal masses during pregnancy. Clin Obstet Gynecol. 2006;49:492–505.
- Kumari I, Kaur S, Mohan H, Huria A. Adnexal masses in pregnancy: A 5 year review. Aust N Z Obstet Gynecol. 2006;46:52–4.
- Aggarwal P, Kehoe S. Ovarian tumours in pregnancy: A literature review. Eur J Obstet Gynecol Reprod Biol. 2011;155:119–24.
- Whitecar P, Turner S, Higby K. Adnexal masses in pregnancy: A review of 130 cases undergoing surgical amangement. Am J Obstet Gynecol. 1999;181:19–24.
- Alalade AO, Maraj H. Management of adnexal masses in pregnancy. The Obstetrician & Gynaecologist. 2017;19:317–25. DOI: 10.1111/tog.12417.
- Dgani R, Shoham Z, Atar E, Zosmer A, Lancet M. Ovarian carcinoma during pregnancy: a study of 23 cases in Israel between the years 1960 and 1984. Gynecol Oncol 1989;33:326–31
- Spencer CP, Robarts PJ. Management of adnexal masses in pregnancy. The Obstetrician & Gynaecologist 2006;8:14–19
- Hakoun, A.M, Aboual-shaar, I, Salloum, M.N. Adnexal masses in pregnancy: An updated review. Avicenna Journal of Medicine. 2017;7(4): 153-157.
- Nick, A, Schmeler, K. Adnexal Masses in Pregnancy. Perinatologycom. [Online] 2010;1(2): 13-19. Available from: http://perinatology.com/perinatology/Volume1-Issue2/Adnexal%20Masses%20in%20Pregnancy.htm [Accessed 20 May 2020].
- Schwartz, N., I.E. Timor-Tritsch, and E. Wang, Adnexal masses in pregnancy. Clin Obstet Gynecol, 2009. 52(4): p. 570-85.
- NaseerA. Https://eposmyesrorg/esr/viewing/indexphp?module=viewing_poster&task=viewsection&pi=119488&ti=394671&si=1388&searchkey=. [Online]. Available from: https://epos.myesr.org/esr/viewing/index.php?module=viewing_poster&task=viewsection&pi=119488&ti=394671&si=1388&searchkey= [Accessed 2014].
- Givens V, Mitchell G, Harraway-Smith C, Reddy A, Maness D, Diagnosis and Management of Adnexal Masses. Am Fam Physician. 2009 Oct 15;80(8):815-820.
- Andreotti R, Timmerman D, Strachowski L M, Froyman W et al. O-RADS US Risk Stratification and Management System: A Consensus Guideline from the ACR Ovarian-Adnexal Reporting and Data System Committee. Radiol 2020 294:1, 168-185
- Naggara, I.T. European journal of radiology. [Online]. Available from: https://www.ejradiology.com/article/S0720-048X(17)30203-6/fulltext#secsect0005 [Accessed 22 may 2017].
- Hannah C. Chang, Shweta Bhatt, and Vikram S. Dogra. Pearls and Pitfalls in Diagnosis of Ovarian Torsion. RadioGraphics 2008 28:5, 1355-1368
- Chiou, S.Y., et al., Adnexal torsion: new clinical and imaging observations by sonography, computed tomography, and magnetic resonance imaging. J Ultrasound Med, 2007. 26(10): p. 1289-301.
- Ssi-Yan-Kai G, Rivain AL, Trichot C, et al. What every radiologist should know about adnexal torsion. Emerg Radiol. 2018;25(1):51‐59. doi:10.1007/s10140-017-1549-8
- LeeEJ, Kwon HC, Joo HJ, Suh JH, Fleischer AC. Diagnosis of ovarian torsion with color Doppler sonography: depiction of twisted vascular pedicle. J Ultrasound Med1998; 17(2): 83–89.
- VijayaraghavanSB. Sonographic whirlpool sign in ovarian torsion. J Ultrasound Med2004; 23(12): 1643–1649.
- McCort J. Ruptured Corpus Luteum with Hemoperitoneum. Radiology 1975 116:1, 65-67
